User:Mr. Ibrahem/Opioid overdose
Toxicity due to excessive opioids / From Wikipedia, the free encyclopedia
An opioid overdose is toxicity due to excessive opioids.[9][3] Examples of opioids include morphine, heroin, fentanyl, tramadol, and methadone.[1][4] Symptoms include insufficient breathing, small pupils, and unconsciousness.[1] Onset of symptoms depends in part on the route by which the opioids are taken.[10] Among those who initially survive, complications can include rhabdomyolysis, pulmonary edema, compartment syndrome, and permanent brain damage.[2][3]
| Opioid overdose | |
|---|---|
| Other names | Narcotic overdose, opioid poisoning |
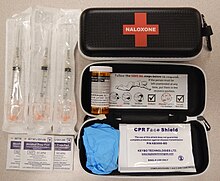 | |
| A naloxone kit as distributed in British Columbia, Canada | |
| Specialty | Emergency medicine |
| Symptoms | Insufficient breathing, small pupils, unconsciousness[1] |
| Complications | Rhabdomyolysis, pulmonary edema, compartment syndrome, permanent brain damage[2][3] |
| Causes | Opioids (morphine, heroin, fentanyl, tramadol, methadone)[1][4] |
| Risk factors | Opioid dependence, use of high doses of opioids, injection of opioids, use with alcohol, benzodiazepines, or cocaine.[1][5] |
| Diagnostic method | Based on symptoms[3] |
| Differential diagnosis | Low blood sugar, alcohol intoxication, head trauma, stroke[6] |
| Prevention | Improved access to naloxone, treatment of opioid dependence[1] |
| Treatment | Supporting a person's breathing, naloxone[7] |
| Deaths | 122,100 (2015)[8] |
Risk factors for opioid overdose include opioid dependence, use of opioids by injection, use of high doses of opioids, mental disorders, and use of opioids together with alcohol, benzodiazepines, or cocaine.[1][11][5] Risk of overdose is particularly high following detoxification.[1] Dependence on prescription opioids can occur from their use to treat chronic pain.[1] Diagnosis of an opioid overdose is based on symptoms and examination.[3]
Initial treatment involves supporting the person's breathing and providing oxygen.[7] Naloxone is then recommended among those who are not breathing to reverse the opioid's effects.[7][3] Giving naloxone into the nose or as an injection into a muscle appear to be equally effective.[12] Among those who refuse to go to hospital following reversal, the risks of a poor outcome in the short term appear to be low.[12] Efforts to prevent deaths from overdose include improving access to naloxone and treatment for opioid dependence.[1]
Opioid use disorders resulted in 122,000 deaths globally in 2015, up from 18,000 deaths in 1990.[8][13] In the United States, over 49,000 deaths involved opioids in 2017.[5] Of those, about 20,000 involved prescription opioids and 16,000 involved heroin.[5] In 2017, opioid deaths represented more than 65% of all drug overdose related deaths in the United States.[5] The opioid epidemic is believed to be in part due to assurances in the 1990s by the pharmaceutical industry that prescription opioids were safe.[4]